Last Updated: March 2, 2026
Hey there, friend. Have you ever poured your heart out to someone close, only to feel like they just didn’t get it? Or maybe their response left you feeling even more alone? I’ve heard stories like this from so many of my readers over the years, and it’s something that hits close to home for me too. Emotional support is that lifeline we all crave during tough times – the kind words, the listening ear, the validation that says, “You’re not alone in this.” But what happens when that emotional support isn’t quite what you need?
In this post, we’re diving into the nuances of emotional support, exploring when it’s empowering and when it might actually hold you back. We’ll look at peer support mental health dynamics, spot toxic relationships signs, and discover ways to build your own inner resilience through self-compassion exercises. Because sometimes, the most reliable emotional support starts from within.
Emotional support isn’t just a buzzword; it’s the foundation of how we navigate life’s ups and downs. Whether it’s a friend checking in after a rough day or a partner holding space for your feelings, good emotional support can make all the difference. But mismatched emotional support – like when someone’s advice feels off-base or dismissive – can leave you spiraling. That’s why understanding emotional support in mental health is key. Let’s break it down step by step, with real insights from research and stories that might feel familiar.

Table of Contents
At a Glance
| Section | Gentle Summary | Key Takeaway (Guilt-Free Note) |
|---|---|---|
| Types of Emotional Support | Explores 4 main types: emotional (empathy/validation), instrumental (practical help), informational (advice), and appraisal (affirmation/feedback). | Mismatches can feel like neglect, but recognizing them validates your needs—it’s okay if what you receive doesn’t fit. |
| Benefits of Strong Emotional Support | Highlights perks like reduced anxiety (e.g., lower cortisol), better coping, resilience, and symptom relief for depression/anxiety. | These show why lacks hurt, but you’re not “missing out”—honor where you are without chasing perfection. |
| How to Provide Effective Emotional Support | 12 low-pressure tips/scripts for active listening, validation, empathy, and boundaries. | Knowing “good” support helps spot absences; use as a mirror for your experiences, not a must-do. |
| Understanding Emotional Support | Defines it as feeling seen/heard; notes reciprocity’s role and prevalence of lacks (e.g., 40–55% adults feel unsupported). | Lacks are common—over 28 million untreated due to this; you’re not alone, and that’s a soft starting point. |
| Power and Pitfalls of Peer Support Mental Health | Benefits like reduced loneliness; pitfalls like mismatches/invalidation. | Peers can validate but also drain—it’s valid to step back without guilt if it doesn’t serve you. |
| Health Pathways: Biological Effects | Lacks raise cortisol/inflammation, shorten telomeres, disrupt sleep, weaken immunity, alter brain chemistry. | Body effects explain why it feels heavy; gentle awareness empowers small, kind steps toward self-care. |
| Comparison: Emotional vs. Other Types | Table contrasting types with descriptions/examples. | Highlights why emotional stands out; mismatches aren’t your fault—use to assess softly. |
| Spotting Toxic Relationships Signs | Patterns like criticism/one-sidedness; impact on anxiety/depression. | Red flags erode support; evaluating without self-blame is a compassionate act. |
| Healthy vs. Toxic Support Table | Contrasts listening/validation/impact. | Gentle tool to reflect on circles—no judgment, just awareness if it feels right. |
| Navigating Emotional Neglect in Relationships | Overlooked feelings build resentment; correlates with depression. | Recognize early; dialogue or pro help is optional—your validity isn’t up for question. |
| Peer Support Challenges | Entanglement/burnout/lack of expertise; frustration from unhelpful interactions. | Good intentions can go awry; moderated spaces help, but pausing is always okay. |
| When to Seek a Therapist for Toxic Relationships | Unbiased unpacking; tools for boundaries/confidence. | Game-changer if signs persist; no rock bottom required—seek when it feels supportive. |
| Embracing Self-Compassion Mental Health Practices | Kindness as buffer; exercises like affirmations/breathing. | Secret weapon for lacks; essential, not selfish—start small, no expectations. |
| Building a Support Network | Reflective steps: journal needs, low-pressure options, diversify/monitor. | Small, guilt-free; one genuine connection > many; self-compassion first if building feels heavy. |
| Case Studies: Extended Reader Scenarios | 3 anonymized stories of lacks (burnout, grief, neurodivergence) and shifts. | Reflections that might resonate—take what helps, leave the rest without apology. |
| Success Stories: Gentle Wins in Rebuilt Support | Quiet shifts like low-key reconnections or therapy-led boundaries. | Possibilities without implying “just do this”—your path looks different, and that’s valid. |
| Real-Life Scenarios: Stories from My Readers | Short anonymized tales of challenges and pivots. | Shows dual edge; empowering when aligned, okay to release when not. |
| Expert Quotes: Insights from the Field | 3 quotes on support’s role, risks, and self-care emphasis. | Validates contrasts; without it, things can turn conflicting—gentle reminders only. |
| Key Statistics on Emotional Support and Mental Health | Prevalence (e.g., 40–55% unsupported); impacts (isolation-suicide links); globals (1/3 youth barriers). | Common, not personal failing; underscores gaps systemically, eases self-blame. |
| Exploring Guilt Free Mind: Categories and Related Reads | 6 categories with linked articles (e.g., self-care rituals, healing betrayal). | Build a personalized path; articles interconnect for ongoing, no-rush support. |
| Related Resources | 5 external tools (helplines, therapy matching, hotlines). | Quiet bridges if needed; always optional, here when you’re ready. |
| Frequently Asked Questions | 11 Qs on lacks/healing/differences/recognition (e.g., for depression, in relationships). | Soft answers for common wonders; everyone’s path unique—include what fits you. |
Understanding Emotional Support: What It Is and Why It Matters
Emotional support is all about feeling seen, heard, and valued. It’s the empathy that helps us process our emotions without judgment. Think of it as the glue that holds relationships together during storms. Research shows that strong emotional support networks can boost resilience and overall well-being. For instance, in one study on adolescents, peers providing caring and understanding – a core part of emotional support – helped reduce stress and promote positive coping (Children (Basel)
. 2025).
But emotional support isn’t one-size-fits-all. It can come from family, friends, or even professionals. The key is reciprocity and genuine understanding. When it’s lacking, people often report higher levels of anxiety and isolation. In surveys, only about 58.5% of teens feel they always or usually get the emotional support they need, which ties directly to poorer mental health outcomes like increased depression symptoms. For adults, the numbers aren’t much better – over 28 million go untreated partly due to perceived lack of emotional support. Globally, including in places like India, one-third of young adults face similar barriers according to World Health Organization data, highlighting a widespread need for better access.

Types of Support: Knowing the Differences
Before we explore what happens when emotional support is lacking, it helps to clearly understand the four main types of social support. Most researchers recognize these distinct categories (House, 1981):
- Emotional Support The focus of this article — empathy, validation, care, love, and reassurance. Example: “That sounds incredibly painful. I’m here with you.” A hug, “I believe in you,” or simply sitting in silence while someone cries.
- Instrumental (Tangible) Support Concrete, practical help that solves a problem. Example: Driving someone to a doctor’s appointment, cooking meals during illness, or helping update a résumé after job loss.
- Informational Support Advice, suggestions, or information that helps solve a problem. Example: “Have you considered this therapist?” or sharing job-search strategies.
- Appraisal Support Affirmation and feedback that helps someone evaluate their own situation or performance. Example: “You handled that meeting with real grace despite how anxious you felt” or “The way you’re protecting your peace right now is really strong.”
The differences matter deeply when emotional support is lacking. If you desperately need emotional validation (“I feel completely overwhelmed”) but receive only instrumental support (“Here’s a to-do list”) or informational support (“Here’s what you should do”), it can feel dismissive or invalidating — even though the other person is genuinely trying to help. This mismatch is one of the most common reasons people feel neglected despite “being supported.”
Research shows that receiving the wrong type of support can sometimes increase distress rather than reduce it.

Benefits of Strong Emotional Support: A Positive Counter to the Gaps
Strong emotional support offers real benefits, like reduced anxiety and better coping—think of it as a quiet buffer against life’s edges. For benefits of emotional support for anxiety, it can lower cortisol levels, easing that constant worry. Studies show those with solid networks report 20-30% less stress, fostering resilience.
Here are a few more gentle perks that highlight why lacks can feel so profound, without any rush to “achieve” them:
- Emotional Regulation Aid: It helps process feelings without overwhelm, potentially reducing mental health symptoms by providing tools for steady responding—no forcing it, just a soft space if available.
- Stress Mediation: Higher emotional support can weaken the impact of perceived stress, aiding coping in tough times and bolstering overall well-being.
- Crisis Management Support: Trusted connections can help navigate daily challenges or decisions, offering a sense of not facing it all alone.
- Resilience Building: It acts as a protective factor, with research linking it to lower depressive symptoms and anxiety in youth—validating how absences might amplify those feelings.
- Health Outcome Improvement: Emotional support may even contribute to longer-term well-being, like reduced mortality risks through structural ties, though this varies gently by context.
- Symptom Reduction in Conditions: For emotional support for depression, it can ease isolation and symptoms, making space for what resonates without expectation.
But here’s the truth: These perks highlight how painful it is when emotional support is lacking. Without it, anxiety might spike, turning small worries into spirals. This contrast validates why addressing gaps matters—it’s not about chasing perfection, but honoring your needs without guilt.
How to Provide Effective Emotional Support: Recognizing What Good Looks Like
Knowing how to provide effective emotional support can help you spot when it’s absent in your own life—it’s like a mirror to reflect on mismatches without self-blame. While our focus here is on what to do when it’s lacking, understanding the “right” way offers contrast, empowering you to validate your experiences or gently guide others if it feels right. Try out these 12 practical tips, drawn from gentle, empathetic approaches, including scripts for active listening.
- Sit with their words. Script: “I’m here to listen—take your time.” This builds trust, but if it’s missing, it can feel dismissing.
- Acknowledge emotions before advice. Script: “That sounds really tough; it’s okay to feel overwhelmed.” Lacking this amplifies isolation.
- Share understanding. Script: “I’ve felt something similar; you’re not alone.” When absent, it leads to self-doubt.
- Encourage sharing. Script: “What does that feel like for you?” Without it, conversations stay superficial.
- Show up consistently. Tip: A simple text like “Thinking of you” matters. Gaps here breed resentment.
- Don’t minimize with “others have it worse.” Script: “Your experience is valid as it is.” This prevents spiraling invalidation.
- Support without burnout. Script: “I care, but let’s talk when I’m fully here.” Ignoring this causes entanglement.
- Check in later. Script: “How are you feeling since we talked?” Lack of follow-up deepens neglect.
- Nod, eye contact, or a hug if appropriate. These amplify words, but silence feels cold.
- Suggest without pushing. Script: “Have you thought about talking to a pro? I’m here either way.” This bridges gaps.
- In partnerships, it’s daily check-ins like “How was your day, really?” When missing, bonds weaken.
- Tailor to backgrounds—some prefer quiet presence over words. Mismatches here highlight unmet needs.
The Power and Pitfalls of Emotional Support in Mental Health
Emotional or Peer support mental health has gained traction as a way for people with shared experiences to lift each other up. It’s that sense of “I’ve been there too” that can make all the difference. Studies highlight how peer support mental health initiatives reduce loneliness and build self-efficacy. For example, in a systematic review, peer support showed small but positive effects on personal recovery, with participants feeling more hopeful and empowered (Psychiatry Online, 2023).

Picture this: Sarah, a 28-year-old dealing with anxiety, joined an online forum for peer support mental health. At first, sharing stories with others who understood her triggers felt liberating. They swapped tips on breathing techniques and daily routines, which helped her manage flare-ups. This kind of emotional support from peers can be incredibly validating, especially when traditional therapy feels out of reach.
However, peer support mental health isn’t without its hurdles. One common issue is mismatched emotional support, where advice doesn’t align with your needs. If a peer downplays your experience because theirs was “worse,” it can invalidate your feelings and worsen isolation. Research on online forums points out how mismatched emotional support can expose users to distressing content or unhelpful responses, leading to disengagement (JMIR Mental Health, 2024).
Health Pathways: The Biological Effects of Lacking Emotional Support
Lacking emotional support isn’t just emotional— it affects your body too. Research from PMC shows pathways where chronic isolation raises cortisol, inflammation, and weakens immunity, linking to higher heart disease risk. Biologically, without emotional support, the stress response stays activated, potentially shortening telomeres and accelerating aging.
More examples: It can disrupt sleep cycles, leading to fatigue and cognitive fog, or weaken the immune response, increasing vulnerability to illnesses. Chronic lack may also alter brain chemistry, reducing serotonin and heightening depression risk. Gentle awareness helps—it’s not your fault, but understanding empowers small steps.
Comparison: Emotional Support vs. Other Types of Support
| Type of Support | Description | Examples | When It Helps | When It Falls Short |
|---|---|---|---|---|
| Emotional Support | Empathy and validation | “I hear you; that’s tough.” | Reduces isolation, boosts mood | If mismatched, feels invalidating |
| Instrumental Support | Practical help | Running errands, cooking | Eases daily burdens | Ignores feelings, leading to resentment |
| Informational Support | Advice or info | Sharing resources | Guides decisions | Overwhelms if unsolicited |
| Appraisal Support | Feedback on coping | “You’re handling this well.” | Builds confidence | Minimizes struggles if not genuine |
This table highlights how emotional support stands out, but lacks can make others feel insufficient.
Spotting Toxic Relationships Signs and Their Impact
Toxic relationships signs often creep up slowly, but they can erode your emotional support system. Look for patterns like constant criticism, emotional manipulation, or one-sided conversations where your needs are ignored. These are red flags that the relationship might be draining rather than supportive.
Take Mike’s experience: He confided in a long-time friend about his job stress, seeking emotional support. Instead, his friend always shifted the talk to their own issues, leaving Mike feeling unheard. This is a classic toxic relationships sign – prioritization of one person’s problems over mutual care. Over time, it led to Mike withdrawing, amplifying his stress.

Toxic relationships signs aren’t just annoying; they harm mental health. Constant negativity can spike anxiety and depression, making it harder to seek genuine emotional support elsewhere. Comparing your pain to someone else who seems to be suffering more only serves to minimize what you are feeling… Comparisons often lead people to think that they can just deal with problems on their own. Rather than reach out for help and support, people are often left feeling that their issues aren’t serious enough to warrant attention (Verywell Mind, 2024). If you’re spotting these, it might be time to evaluate if the connection is worth the toll.
Healthy vs. Toxic Support: A Comparison Table
| Aspect | Healthy Emotional Support | Toxic Support Signs |
|---|---|---|
| Listening | Active, empathetic | Dismissive or interrupting |
| Validation | Affirms feelings | Minimizes or compares |
| Reciprocity | Mutual care | One-sided |
| Impact | Builds resilience | Increases isolation |
Use this to gently assess your circles.
Navigating Emotional Neglect in Relationships
Emotional neglect in relationships is like a silent thief – it steals your sense of security without obvious conflict. It’s when your partner or friend consistently overlooks your feelings, leaving you to handle everything alone. This lack of emotional support can build resentment and deepen loneliness.
Consider Lisa, who felt emotional neglect in her marriage. Her husband was great with practical help but dismissed her worries as “overthinking.” Over months, this emotional neglect in relationships made her question her own validity, leading to self-doubt and withdrawal. Studies show that emotional neglect in relationships correlates with higher depression rates, as it chips away at your emotional foundation.
The key? Recognize it early. If conversations feel superficial or your vulnerabilities are met with indifference, it’s a sign emotional support is missing. Addressing emotional neglect in relationships starts with open dialogue, but if that fails, professional help can guide the way.

Peer Support Challenges: When Good Intentions Go Awry
Peer support challenges arise even in well-meaning groups. The weakness is represented by peers both being too involved and focused on personal interest or by peers lacking expertise and knowledge (Science Direct, 2023). Culture, language barriers, drop-out rates, securing sustainability, and peers’ lack of time and commitment are regarded as threats to peer support. For instance, emotional entanglement – where peers get too involved – can trigger burnout or reawaken old traumas. Receiving empathy from partners also was related to conflict escalation. Eventually, it burns you out (MDPI, 2026). A full 56% of those who had received this type of empathy reported avoiding their adversaries (The Conversation, 2020). In one review, peer supporters reported fatigue from over-identification with others’ struggles (Fam Pract, 2022)
Another peer support challenge is the lack of expertise. Untrained peers might offer advice that doesn’t fit, creating mismatched emotional support. If you are the one offering support, you’ll need to maintain clear professional boundaries. This means avoiding over-involvement in participants’ personal lives, refraining from dual relationships and keeping yourself from spiralling or dawing parallels (Quest Behavioral Health). This can spiral into frustration, as seen in forums where users feel more distressed after unhelpful interactions.
I’ve had readers share how peer support challenges in online groups led them to step back. One woman described feeling neglected when her posts went unanswered, exacerbating her isolation. Peer support challenges like these highlight the need for moderated spaces and clear boundaries.
When to Seek a Therapist for Toxic Relationships
If toxic relationships signs persist, consulting a therapist for toxic relationships can be a game-changer. Therapists provide unbiased emotional support, helping you unpack patterns and rebuild confidence. They’re trained to spot dynamics you might miss, like subtle manipulation or codependency.

For example, after recognizing toxic relationships signs in her friendship circle, Emily sought a therapist for toxic relationships. Through sessions, she learned to set boundaries and prioritize her well-being. Research supports this – therapy for such issues reduces symptoms by offering tools for healthier connections (Better Help, 2026).
Don’t wait for rock bottom. If emotional support from peers feels consistently off, a therapist for toxic relationships can help you navigate the exit or repair.
Embracing Self-Compassion Mental Health Practices
Self-compassion mental health is your secret weapon when external emotional support falters. It’s treating yourself with the kindness you’d offer a friend – no judgment, just understanding. Studies link self-compassion mental health to lower burnout and higher resilience, acting as a buffer against stress (Psychol Res Behav Manag, 2022)
Try these self-compassion exercises: Start with a daily affirmation like “I’m doing the best I can.” Or practice mindful breathing: Inhale kindness, exhale self-criticism. One reader told me how self-compassion exercises helped her after feeling neglected in a group – she journaled her wins, shifting from external validation to inner peace.
Self-compassion mental health isn’t selfish; it’s essential. When peer support challenges arise, turning inward builds lasting emotional support.
If this resonates, I created a small, printable set of gentle permission slips you can keep close on days when emotional support feels far away. No pressure to read them all at once, or even to use them every day. They’re just soft reminders that your feelings are valid, even when no one else is meeting them right now.

Building a Support Network: Gentle Steps When Starting Feels Hard
Building a support network doesn’t have to be overwhelming—it’s about small, guilt-free steps, especially when past lacks make trust tricky. Start by reflecting: What kind of emotional support do you need? Journal prompts can help, like “What made me feel seen before?”
Next, explore low-pressure options: Join moderated online communities for peer support mental health, where boundaries are clear. Or reconnect with one trusted person—send a simple message: “Hey, I’ve been thinking about you; how are things?” If that feels too much, begin with professionals, like a therapist for toxic relationships.
Diversify: Mix family, friends, and pros. Set expectations gently: “I appreciate your listening ear.” Monitor for mismatches—if emotional neglect in relationships creeps in, it’s okay to pause. Common barriers include emotional concerns (e.g., anxiety), time constraints, and lack of motivation (Science Direct, 2023). Over time, this builds resilience; studies show diverse networks reduce isolation by 25-40%.
Remember, it’s not about quantity; one genuine connection trumps many shallow ones. If building feels heavy, that’s valid—start with self-compassion mental health first.
Case Studies
To deepen understanding without overwhelm, here are three extended, anonymized case studies from my readers—gentle reflections on when emotional support lacked and what shifted. These aren’t blueprints, just stories that might resonate.
The burnout case of Alex
Alex, 42, navigated burnout in a high-stress job. He sought emotional support from colleagues in a peer support mental health chat, sharing exhaustion from deadlines. But responses focused on “push through” advice, a classic mismatched emotional support that minimized his fatigue. It spiraled his self-doubt, leading to sleepless nights and withdrawal. We expected that support from friends would explain the link between being bullied and vulnerability to mental health issues, but it did not (Psychology Today, 2026). Recognizing toxic relationships signs like one-sided convos, Alex stepped back. He tried self-compassion exercises, journaling “This tiredness makes sense,” and sought a therapist for toxic relationships. Over months, he rebuilt with a small, understanding friend group—gentle check-ins without pressure. Now, he honors low-energy days without guilt.

Maria and her grief
Maria, 31, faced grief after loss. Family offered instrumental help but dismissed her sadness as “lingering too long,” emotional neglect in relationships that deepened isolation. How to recognize lacking emotional support? For her, it was superficial talks avoiding feelings. This triggered anxiety spirals, questioning her validity. Maria pivoted to online forums, but peer support challenges like comparisons worsened it. Gently, she explored emotional support for depression through books and therapy.
A key shift: Daily affirmations and a support network of one empathetic cousin. Today, she validates her pace, finding quiet strength.
Jordan and his struggle with neurodivergence
Jordan, 25, dealt with neurodivergence and overwhelm. Friends’ “just relax” minimized triggers, mismatched emotional support amplifying shame. Extended isolation followed, but recognizing how to recognize lacking emotional support—indifference to needs—prompted change. Jordan built a network via moderated apps, incorporating self-compassion mental health. Success came slowly: A therapist helped unpack toxic relationships signs, leading to boundaries. Now, with rebuilt connections, Jordan feels seen without exhaustion.
Success Stories: Gentle Wins in Rebuilt Support
To balance the lacks, here are soft success stories from readers—moments where rebuilding emotional support felt possible, without implying “just do this.” These aren’t triumphs over struggle, but quiet shifts that honored their pace.
One reader, after mismatched emotional support in family, started with self-reflection: “What small connection feels safe?” She reached out to an old friend with a low-key text, leading to gentle walks where listening flowed naturally. Over time, this rebuilt trust, easing her isolation without pressure.
Another shared rebuilding after peer support challenges: Post-burnout, he joined a moderated group, setting boundaries early. A consistent check-in buddy offered validation, turning spirals into shared understanding. It wasn’t instant, but it validated his needs, fostering resilience.
A third found emotional support for depression through therapy, then extended to a hobby meetup. One empathetic conversation sparked ongoing support, reminding her “you’re not alone.”
Expert Quotes: Insights from the Field
As one study notes, “Emotional support involves interaction partners providing caring and understanding. Because emotional support given implies that a person is esteemed and accepted, it has also been referred to as esteem support” (Front Psychol, 2022). This highlights how true emotional support fosters acceptance, but without it, relationships can turn conflicting.
Another insight: “Peer support can provide unique benefits but also poses risks like emotional fatigue”
From a third: “Lacking support correlates with poorer health outcomes, emphasizing self-care’s role” (BMJ Open, 2022).
Key Statistics on Emotional Support and Mental Health
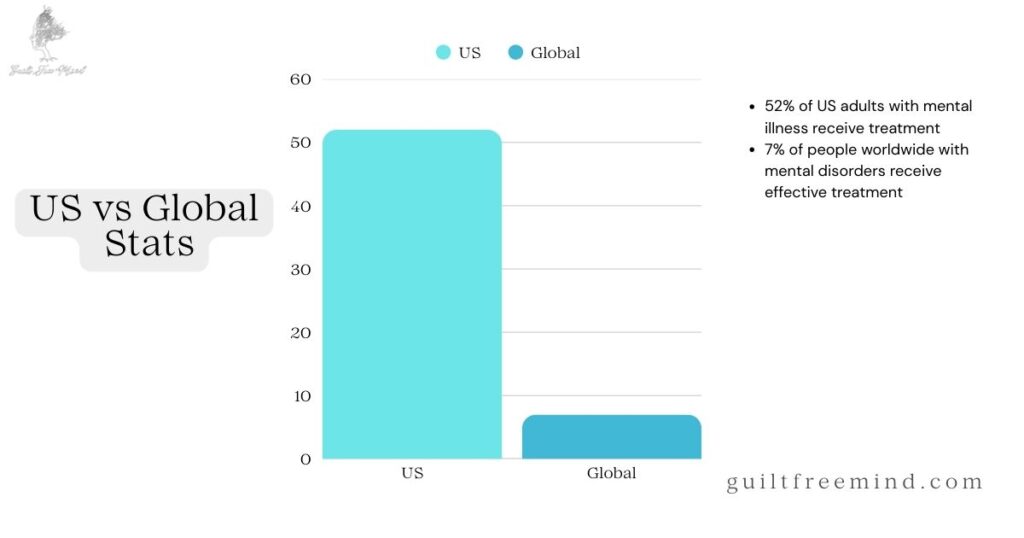
Data paints a clear picture: In recent reports, over 129 million people live in areas with mental health professional shortages, making peer emotional support crucial yet often insufficient. Untreated mental illness affects more than 28 million adults, partly due to inadequate emotional support. Programs incorporating peer support show promising results – participants are 53% more likely to return to work and experience a 30% drop in hospital readmissions. Costs can decrease by 24-47%, with emergency visits falling from 21% to 9%. For teens, only 59% report consistent emotional support, linking to higher anxiety and depression (APA, 2025).
More US figures from APA 2025: 40% of adults feel unsupported emotionally, rising to 55% among young adults. Suicide rates link to isolation in 30% of cases. Additional sources: 54% of U.S. adults felt isolated often or sometimes (APA Stress in America 2025). 5% of U.S. adults regularly experience depression (CDC, 2026). 23.40% of U.S. adults experienced any mental illness (MHA, 2025). Globally, contrasts show India with 35% youth facing barriers (WHO), while Europe averages 25%. These underscore the gaps.
Explore More on Guilt Free Mind
Whether you’re learning to sit with the ache of missing emotional support, gently naming what doesn’t feel safe in your relationships, or quietly rebuilding trust starting with yourself, these resources from Guilt Free Mind support your journey—one compassionate breath at a time.
🧘♀️ Self-Care and Wellness
Discover soft daily rituals that help you feel held when external support is inconsistent—gentle movement, grounding practices, sensory soothing, and restorative pauses that remind your nervous system you are safe enough to rest.
🧠 Understanding Personality Disorders
Explore how certain relational patterns (dismissal, minimization, emotional invalidation) can echo traits of personality disorders. These articles offer compassionate insight without blame, helping you recognize dynamics and protect your peace with clearer boundaries.
🎨 Creative Healing and Therapy
Use expressive outlets—journaling, art, handwriting analysis, somatic drawing, or voice memos—to give shape to feelings that weren’t received or validated by others. Turn unspoken hurt into something you can witness and hold with kindness.
💡 Mindful Productivity and Focus
Learn to protect your energy when emotional neglect leaves you foggy or scattered. Gentle techniques for setting micro-boundaries, saying no without guilt, and returning to presence help you reclaim focus without forcing productivity on low-support days.
💪 Emotional Recovery and Resilience
Build inner anchors that don’t depend on anyone else showing up perfectly. These pieces guide you through grieving unmet needs, releasing shame around wanting connection, and slowly strengthening the quiet resilience that grows from self-trust.
😌 Stress, Anxiety, and Depression Toolkit
Find immediate, body-first tools to lower the intensity when loneliness or invalidation spikes anxiety or deepens low mood—breath resets, cold exposure options, grounding anchors, and micro self-compassion practices that create small pockets of relief without needing anyone else to “fix” it.
Related Resources
- APA Helpline: Call 1-800-273-TALK for immediate emotional support.
- BetterHelp: Online therapy matching for toxic relationships.
- NAMI Hotline: 1-800-950-NAMI for peer support mental health resources.
- Crisis Text Line: Text HOME to 741741 for quick validation.
- WHO Mental Health Resources: Global tools for anxiety management.
Conclusion
If anything here landed softly today—even just one sentence or one quiet moment of recognition—thank you for letting it in.
You don’t have to change anything right now.
You don’t have to rebuild anything overnight.
You’re allowed to sit with what you’ve felt, breathe, and come back when (or if) it feels right.
Whenever you want more gentle company on this path, I’m here in a few quiet places:
🖤 YouTube – Guilt Free Mind
Short, validating videos on nervous system regulation, self-compassion practices, boundary-setting without guilt, and small ways to feel a little less alone when support has been hard to find.
Subscribe if it feels helpful—no pressure, just a soft space to return to.

💌 GuiltFreeMind.com
More articles, reflection prompts, and free printables are always here waiting—no login, no rush. Save this page, bookmark what resonates, or come back whenever your energy allows.
If you’d like to share a small piece of your story in the comments below (anonymously or not), know that your words might quietly help someone else feel less alone today. But only if it feels safe and kind to you.
You’re not behind.
Not broken.
You are doing what you can—and that’s enough.
With gentleness always,
Shruti
Frequently Asked Questions
Without emotional support, feelings of isolation can intensify, leading to heightened stress, anxiety, or depression. It might make daily challenges feel overwhelming, but remember, building internal resilience through self-compassion mental health practices or seeking professional help can fill that gap.
Healing starts with acknowledging your needs – try self-compassion exercises like journaling or mindfulness. Connect with supportive communities or a therapist for toxic relationships if past ones were harmful.
Lack of support can erode self-esteem, increase vulnerability to mental health issues, and lead to withdrawal from relationships. It affects people differently, but fostering self-reliance and diverse connections can mitigate these effects for all.
Mental support often involves practical advice or cognitive strategies for problem-solving, while emotional support focuses on empathy and validation of feelings. Both are vital, and they can overlap in peer support mental health settings.
Start softly: “I’m going through something and could use a listening ear—no advice needed.” Be specific if comfortable, like “Can we talk about my anxiety?”
No—some emphasize community sharing, others quiet presence. Mismatches can feel neglecting.
It’s okay to step back; pivot to self-compassion mental health without guilt.
Look for signs like dismissed feelings, one-sided talks, or persistent loneliness—it’s valid to notice.
Ready to Build Your Emotional Toolkit? Let’s Connect!
If this resonated, don’t stop here – dive deeper into emotional support strategies on my YouTube channel, Guilt Free Mind. Subscribe for videos on self-compassion exercises, spotting toxic relationships signs, and overcoming peer support challenges. Drop a comment sharing your story; your insight could be the emotional support someone needs today. Share your story below in the comments—what’s one time emotional support fell short for you? And if you’re ready for personalized guidance, reach out via the contact form on guiltfreemind.com – let’s make your mind guilt-free together!
About the Author
Dr. Shruti Bhattacharya is the founder and heart of Guilt Free Mind, where she combines a Ph.D. in Immunology with advanced psychology training to deliver science-backed mental health strategies. Her mission is to empower readers to overcome stress, anxiety, and emotional challenges with practical, evidence-based tools. Dr. Bhattacharya’s unique blend of expertise and empathy shapes her approach to wellness:
- Academic & Scientific Rigor – Holding a Ph.D. in Immunology and a Bachelor’s degree in Microbiology, Dr. Bhattacharya brings a deep understanding of the biological foundations of mental health, including the gut-brain connection. Her completion of psychology courses, such as The Psychology of Emotions: An Introduction to Embodied Cognition, from University of Cambridge enhances her ability to bridge science and emotional well-being.
- Dedicated Mental Health Advocacy – With over 15 years of experience, Dr. Bhattacharya has supported hundreds of individuals through online platforms and personal guidance, helping them navigate mental health challenges with actionable strategies. Her work has empowered readers to adopt holistic practices, from mindfulness to nutrition, for lasting resilience.
- Empathetic Connection to Readers – Known for her compassionate and relatable voice, Dr. Bhattacharya is a trusted guide in mental health, turning complex research into accessible advice. Her personal journey as a trauma survivor fuels her commitment to helping others find calm and confidence.
- Lifelong Commitment to Wellness – Dr. Bhattacharya lives the principles she shares, integrating science-based habits like balanced nutrition and stress management into her daily life. Her personal exploration of mental health strategies inspires Guilt Free Mind’s practical, reader-focused content.
- Wolday, M., & Montazeri, A. (2024). Between support and risk: The dual role of peer relationships in adolescents’ mental health. Frontiers in Psychology, 15, Article 1265082.
- Fu, R., Chen, X., Wang, Y., & Li, B. (2022). The effectiveness of peer support in personal and clinical recovery: Systematic review and meta-analysis. Psychiatric Services, 73(4), 427–435.
- De Mol, J., Buysse, A., & Colpin, H. (2022). The benefits and challenges of established peer support programmes for patients, informal caregivers, and healthcare providers: A systematic review. BMC Health Services Research, 22(1), Article 1176.
- Prescott, J., Hanley, T., & Gomez, R. (2024). Understanding the impacts of online mental health peer support forums: Realist synthesis. JMIR Mental Health, 11, e55750.
- Raypole, C. (2023). Understanding toxic friendship: Identifying toxic relationships and peer pressure. BetterHelp.
- Shalisko, M., & Shalisko, V. (2022). Scoping review to evaluate the effects of peer support on the mental health of young adults. BMJ Open, 12(8), e061336.
- Kotera, Y., & Ronaldson, A. (2022). The benefits of self-compassion in mental health professionals: A systematic review of empirical research. Psychology Research and Behavior Management, 15, 3649–3666.
- Reis, H. T., Lee, K. Y., O’Toole, A., Feng, Q., & Clark, M. S. (2023). Effects of supportive and conflicting interactions with partners and friends on emotions: Do the source and quality of relationships matter? Journal of Personality and Social Psychology, 124(1), 181–199.
- Cherry, K. (2024). Why comparing feelings isn’t helpful. Verywell Mind.
- Gable, S. L. (2019). The dark side of supportive relationships. The Conversation.
- Mikolajczak-Degrauwe, K., Slimmen, S. R., Gillissen, D., de Bil, P., Bosmans, V., Keemink, C., Meyvis, I., & Kuipers, Y. J. (2023). Strengths, weaknesses, opportunities and threats of peer support among disadvantaged groups: A rapid scoping review. International Journal of Nursing Sciences, 10(4), 587–601.
- Morales-Ortiz, J., Eiroa-Orosa, F. J., López-García, J. J., & Pereñíguez, M. D. (2026). Between lived experience and professionalisation: Can personal assistance redefine peer support in mental health? Healthcare, 14(3), Article 346.
- McVay, S., & Santo, J. (2026). Rethinking the power of peers during adolescence. Psychology Today.
- Quest Behavioral Health. (n.d.). What is peer support in mental health and how it helps. Quest Behavioral Health. Retrieved February 13, 2026, from
- American Psychological Association. (2025). U.S. teens need far more emotional and social support. Monitor on Psychology, 56(3), 24–29.
- Batchelor, R., & Taylor, M. D. (2023). Experiences and perspectives of peer support among young adults with epilepsy. Epilepsy & Behavior Reports, 21, Article 100590.

